Stem cells were discovered in cord blood in 1978, and the first cord blood transplant followed ten years later. Since then, more than 40,000 cord blood transplants have been performed around the globe.
A stem cell transplant, or immune system reconstitution, is used to replace maligned cells or invigorate the system’s production of new healthy cells. This may be needed when someone undergoes radiotherapy or chemotherapy to treat a cancer of their blood or immune system or when the person has blood or immune system deficiency. In addition to renewing healthy cells into the body, in some cases, the transplanted cells can attack the cancer or malignancy itself.
Stem cell transplants are not uniform. Variances depend on the disease being treated, the state and health of the patient, the physician conducting the therapy and the type of transplant (autologous [self] versus allogeneic [donor]) that is going to be performed.
Transplant versus Transfusion
Let’s draw a clear line on the difference between transfusion and transplantation. Transfusion is the introduction of new cell lines into the body, often to supplement losses, such as when a loss of blood has occurred and new matching blood is provided to the patient. A transplant is the replacement of old cell lines with new cell lines; these news cells are transplanting the old cells. As stem cell infusions are used to replace the current supply of blood and immune system cells, it is called a stem cell transplantation.
Stem Cell Source
The source of the stem cells is determined by a few different factors: Availability is limited by access to donor cells and the person’s own ability to provide stem cells. HLA proteins are the compatibility markers that help determine how closely the donor’s and recipient’ cells match. Low matches increase the probability and severity of graft-versus-host disease, which is when the person’s own immune system attacks the body.
With more than 7,000 currently known HLA protein types, perfect matches are rare and often only found when the donor is able to use his or her own stem cells. Cord blood stem cells are always a perfect match for the child and have many advantages over similar stem cells from other sources. If the patient does not have stored cord blood, the patient may be able to acquire and use stem cells from the bone marrow or peripheral blood as an alternative. If the patient is able to use his or her own stem cells, it is called an autologous transplant, or autotransplant.
Unfortunately, the patient’s health and ability to provide his or her own bone marrow or peripheral blood stem cells or the health of the stem cells themselves may limit transplantations to third-party donors, and finding even a partial-match third party donor can be difficult. If the patient is able to find matching donor, it will be an allogeneic transplant, or allotransplant.
Stem Cell Transplant Conditioning
If suitable stem cells are found, the patient undergoes a series of treatments leading up to transplantation. This is called the conditioning stage. For lymphomas and leukemias, either chemotherapy or radiotherapy or a combination of is used to destroy the diseased cells. This may be performed in conjunction with a total body irradiation (TBI), which suppresses or lowers the immune system and helps prevent graft-versus-host disease. The use of TBI can be dependent on how closely the donor’s cell matches the recipient’s cells in allogeneic transplantations. In autologous transplantations, like a cord blood transplant, TBI may not be utilized because of how well the stem cells match.
Stem Cell Transplantation
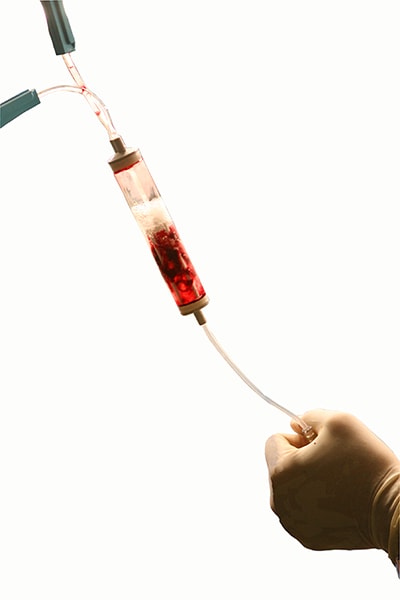 The cord blood is infused through IV right into the patient’s blood supply.
The cord blood is infused through IV right into the patient’s blood supply. Performed within a few days of the conditioning, the cord blood transplantation itself is rather simple and is much like the transfusion of blood. The cord blood stem cells have already been isolated during cord blood processing prior to cryo-preservation. These stem cells are thawed in 37 degree water bath, tested for viability and then infused through intravenous therapy (IV) right into the patient’s blood supply.
In the body, the cord blood stem cells migrate to the center of the bone. In the bone marrow, these stem cells start to produce new, non-diseased blood and immune system cells. In autologous stem cell transplants, like a cord blood transplant, the grafted white blood cells can actually start to attack the cancer and aid recovery. This is something known as graft versus tumor.
Recovery
While the conditioning and transplantation processes may get the most attention, it is the work by the doctors post-transplant that can be the most extensive.
As the body’s immune system has been wiped out, the patient is in a precarious position until the immune system can meet minimum viable strength. It can take three or four weeks for the new, healthy stem cells to reach a number suitable to protect the body. This may require the use of anti-rejection drugs to help the body accept the new cells and growth factors such Granulocyte colony-stimulating factor (G-CSF) to aid stem cell’s asymmetric division. Until that time, the patient may have to reside in a sterile room and be put on a low-microbial diet to decrease the risk of infection. To keep the body functioning properly, the patient may also undergo red blood cell and platelet infusions.
Measuring recovery can be difficult, but a standard is an absolute neutrophil count of 500 across three consecutive days. Neutrophils are the most plentiful type of white blood cell in your immune system and are used to measure the overall health of your system’s ability to fight pathogens. When a patient has an ANC of fewer than 500—a condition called neutropenia—they are at a greater risk of infection. It may take at four weeks to reach an ANC of 500 but still longer to fully recover to an ANC of more than 8,000.
A type of cord blood–processing method has been shown to lead quicker engraftment when the patient is in the precarious stage of neutropenia.
Learn More Here