Why the processing method for cord blood matters
The type of processing method being used doesn’t always enter the conversation on cord blood banking—but it should. Confusion can arise from the term processing, which cord blood banks use as a blanket description of everything that happens once the cord blood has arrived at their facilities.
It is especially good idea to understand how cord blood is processed because there are a number of different processing methods available. The processing method has a large impact on the quality of the collection, which can ultimately lead to a different outcome if it is used in a transplantation. Most cord blood banks offer their customers no choice when it comes to the processing method their babies’ cord blood will undergo. At Cryo-Cell, we give parents two options. We have our standard and a premium processing methods. The former has been the time-tested industry standard since 1988, and the latter is a relatively new type of processing that has been proven better than the other methods in clinical studies. We are the only private cord blood bank to invest and thus be able to offer this premium processing method.
Processing overview
Once the collection kit is received in the laboratory, the processing begins by testing the mother’s blood for infectious disease as required by federal regulations. At Cryo-Cell, we also aliquot a portion of the mother’s blood and freeze it in case future testing is ever required.
Next, a sample of the baby's cord blood is taken for testing purposes. Small samples of the baby's cord blood will actually be taken throughout the process and tested to guarantee quality and verify sterility.
Then, the cord blood is processed. It is mixed with the processing agent, suspended and centrifuged, dividing it into its constituent parts. This is how the stem cells are separated and collected.
Lastly, the cord blood is cryo-preserved. It is slowly lowered to the requisite temperature and preserved in the vapor stage of liquid nitrogen.
How is cord blood processed?
 Two objectives in cord blood processing: remove red blood cells and capture stem cells
Two objectives in cord blood processing: remove red blood cells and capture stem cells
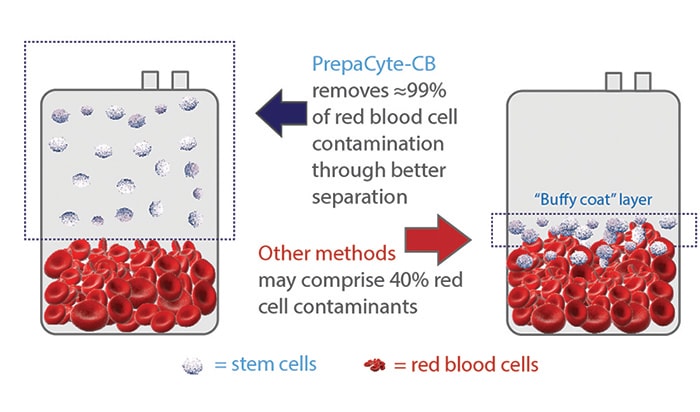
Cord blood is processed not only to prepare it for cryo-preservation but also to get it ready for future transplants. Many parents may be surprised to learn that doctors want the stem cells found in the cord blood but not the red blood cells themselves. The red blood cells (RBCs) can inhibit treatments or cause further complications. The key for processing cord blood is to separate and to extract a high volume of the stem cells while significantly reducing the volume of the collection and the number of red blood cells.
To do this, the cord blood is separated into a layer of RBCs, a layer of plasma, and an in-between layer known as the buffy layer. The buffy layer contains the white blood cells and the stem cells. The type of processing method used can help better separate the cord blood into these three parts, allowing for easier extraction of more stem cells.
Processing also prepares the collection for cryo-preservation. To prevent the cell membranes from rupturing, scientists add a cryo-protectant. Dimethyl sulfoxide (DMSO) is considered the standard choice in the cryo-preservation field and is used by us and other cord blood banks. Ice crystals form when something freezes. In the case of freezing a cell suspension, ice crystals can form and puncture the cell membrane, causing the cell to die. DMSO protects the cells by interfering with the formation of ice crystals. It also solubilizes the cell membrane to a point that makes it less prone to being punctured. (Imagine the difference in trying to puncture a mostly deflated balloon and a fully inflated one.)
The cord blood collection is then brought slowly down to freezing temperatures through a process called controlled-rate freezing, or slow programmable freezing. This will help ensure the cord blood stem cells don’t go inactive or stop functioning correctly. At Cryo-Cell, the collection is lowered to its final temperature incrementally and then stored in vapor-phase nitrogen at −190 degrees Celsius, or −310 degrees Fahrenheit. It is recommended to store cord blood at a temperature below −170 degrees Celsius.
Which processing method is best?
PrepaCyte-CB®

PrepaCyte-CB is Cryo-Cell International's premium processing method. It is a superior type of processing method that greatly enhances parents' return on investment because clinical transplant data point to better engraftment times and treatment outcomes. Cryo-Cell holds the exclusive license to provide and manufacture this technology and makes it available to other cord blood banks for the betterment of the entire industry.
PrepaCyte-CB leads to a better separation by sedimentation of the red blood cells while keeping the white cells suspended in the plasma. This provides less crossover of the red and white cells because they aren’t sitting on top of one another. The plasma–white cell suspension is then pulled away from the red cell layer, and the white cells are then separated from the plasma. Because of the physical difference in separation, Cryo-Cell is able to capture more stem cells while reducing the red cells up to 99%. This equates to more stem cells in every collection.
Hetastarch® (HES)
HES is the name given to the manual method of using Hetastarch® to separate the plasma and the buffy coat containing the white cells from the red blood cells. This processing method has been the industry standard since 1988, and thousands of transplants using HES-processed cord blood have been successful. HES is Cryo-Cell International's standard method for processing cord blood, and it is also the sole processing method used by Viacord®, Americord® and LifebankUSA®.
AutoXpress® (AXP)
Launched in 2006, AutoXpress (AXP) is an automated cord blood processing method designed to lower the cost of processing cord blood and to limit the need for human intervention. It uses optical detection to direct separated components to their respective containers.
There is a drawback to the AXP processing method because of its automated nature and the way the buffy layer and layer of red blood cells overlap to some degree. In order for the AXP machine to acquire more white cells (harvest the buffy coat), it must collect more red cells because the layers are in contact with each other. This in turn raises the total amount of red cells in the final product. If they want to lower the amount of red cells, they will also negatively impact the number of white cells harvested.
AXP is the sole processing method for Cord Blood Registry®.

Sepax®
Sepax was launched in 2008 and is similar to AutoXpress in that it, too, is an automated processing method that uses a light to detect the separation between components. As such, it also suffers from the drawbacks found in the AXP system. Sepax can also use the hydroxyethyl starch agent used in HES processing for a better division between layers.
Processing Method Engraftment Times
How do you judge the success of a cord blood–processing method? With a stem cell transplant, it is the time to engraftment. Engraftment is when the infused stem cells start to introduce new, healthy cells into the blood stream. When chemotherapy or other methods that affect the immune system are utilized in treatment, a person’s immune system will not be able to defend the body against pathogens. The faster the stem cell engraftment, the less risk there is for any life-threatening complications or infections to affect the patient.
In a recent study performed by the St. Louis Cord Blood Bank, patients infused with PrepaCyte-processed stem cells recovered 4 days more quickly than the next-closest processing method (from 20 days to 16 days).
The following table breaks down how well the different cord blood–processing method have performed:
| Processing Method |
Days to Recovery* |
Public Data Source |
Private-Equivalent |
| Prepacyte-CB |
1655 |
St. Louis Cord Blood Bank |
Cryo-Cell |
| HES |
2055 |
St. Louis Cord Blood Bank |
Viacord®, Cryo-Cell |
| AutoXpress® (AXP) |
2056 |
New York Cord Blood Center |
Cord Blood Registry® (CBR) |
| Sepax |
2157 |
Duke University Medical Center |
Cord:Use® |
| HES/Sepax |
21.558 |
Bloodworks |
EverCord |
| HES/Sepax |
2559 |
ClinImmune Labs |
Caricord |
*Recovery time is the median time to reach a absolute neutrophil count (ANC) of 500.
Learn more about the PrepaCyte-CB difference by following the link below